Increases monoamine release (DA > NE> > 5-HT). Treatment specificities in children and for each of the three conditions will be discussed last. First we will review the most commonly used medications across all conditions. In this publication, we will use the DSM-5 classification as a guideline because there is no evidence that the pathophysiology or therapeutic response is substantially different for hypersomnia with or without SOREMPs on the MSLT. In the ICSD3, narcolepsy caused by hypocretin deficiency is called “type 1 narcolepsy” while other hypersomnias (not likely due to hypocretin abnormalities) will stay subdivided into “type 2 narcolepsy” in the presence of a positive Multiple Sleep Latency Test (MSLT) with multiple Sleep Onset REM periods (SOREMPs) vs idiopathic hypersomnia otherwise (for more detail see American Psychiatric Association ). This last group is the most challenging and the most frequent diagnosis.Ī similar revised International Sleep Disorder Classification, 3rd edition (ICSD3) is also being finalized and will use a similar framework to that of the DSM-5 with minor differences. 
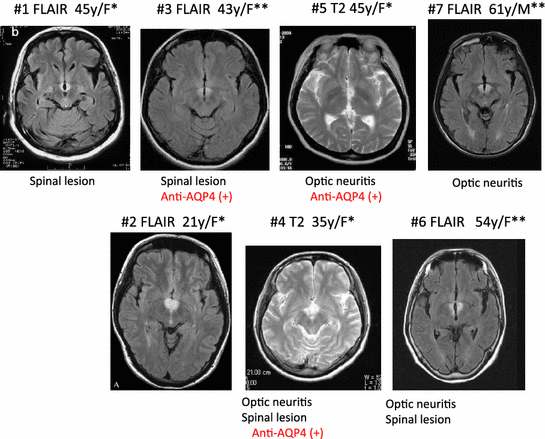
Guidelines are provided based on the literature and personal experience of the author.Īccording to the Diagnostic and Statistical Manual of Mental Disorders, 5th edition (DSM-5) currently being finalized, syndromes with primary hypersomnolence can be practically divided into 3 groups: 1) narcolepsy caused by hypocretin (orexin) deficiency, a disorder associated with Human Leukocyte Antigen (HLA) marker DQB1*06:02 and believed to be autoimmune (almost all cases with cataplexy), 2) Kleine-Levin Syndrome (KLS), and 3) syndromes with hypersomnolence unexplained by hypocretin abnormalities (generally without cataplexy). Kleine-Levin Syndrome is usually best left untreated, although lithium can be considered in severe cases with frequent episodes. As cause and evolution are unknown in these conditions, it is important to challenge diagnosis and therapy over time, keeping in mind the possibility of tolerance and the development of stimulant addiction. Preferably, therapy should be conservative (such as modafinil, atomoxetine, behavioral modifications), but it may have to be more aggressive (high-dose stimulants, sodium oxybate, etc.) on a case-by-case, empirical trial basis. 
Treatment for other syndromes with hypersomnolence is more challenging and less codified. 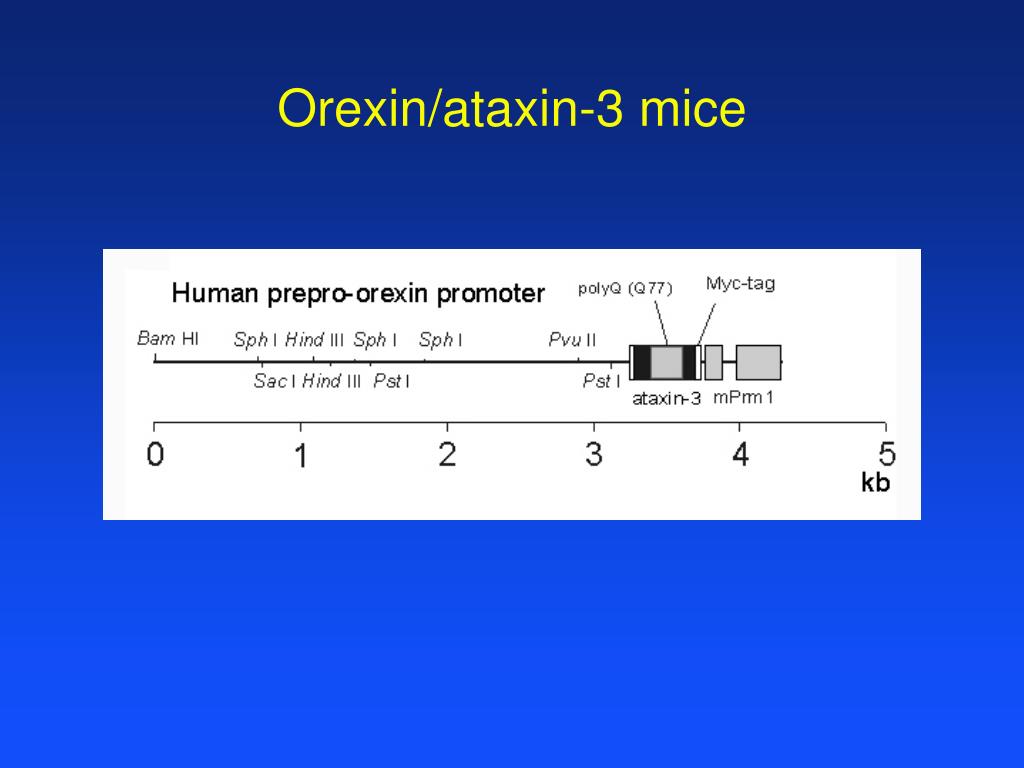
Detailed knowledge of the pharmacological profile of each compound is needed to optimize use. These therapies are almost always needed, and the risk-to-benefit ratio is clear, notably in children. The treatment of narcolepsy/hypocretin deficiency is well-codified, and involves pharmacotherapies using sodium oxybate, stimulants, and/or antidepressants, plus behavioral modifications. These diagnoses are only made after eliminating sleep deprivation, sleep apnea, disturbed nocturnal sleep, and psychiatric comorbidities as the primary cause of daytime sleepiness. Non hypocretin-related hypersomnia syndromes are diagnoses of exclusion. Klein-Levin Syndrome, a periodic hypersomnia associated with cognitive and behavioral abnormalities, is also considered a separate entity with separate therapeutic protocols. New classifications now distinguish narcolepsy/hypocretin deficiency (also called type 1 narcolepsy), a lifelong disorder with well-established diagnostic procedures and etiology, from other syndromes with hypersomnolence of unknown causes. Narcolepsy and other syndromes associated with excessive daytime sleepiness can be challenging to treat. 
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
